What is Chronic Venous Insufficiency (CVI)?
Under the influence of gravity, blood faces a challenge returning from the feet to the heart. Walking helps as the calf muscles squeeze the veins, pushing the blood upwards. Veins also have valves that prevent backflow. If leg veins or valves are damaged or blocked, they can't efficiently return blood to the heart, resulting in Chronic Venous Insufficiency.
- Standing painA person with CVI may experience a ‘bursting and burning’ pain when first standing in the morning, this is caused when blood rushes at speed into the weakened veins. Also, a dull ache or heaviness can develop in the legs when standing.

- SwellingA common sign is swelling of the legs, particularly below the knee. This swelling can become more pronounced when sleeping in a seated position, as it contributes to increased blood pooling and may even lead to skin damage over time.
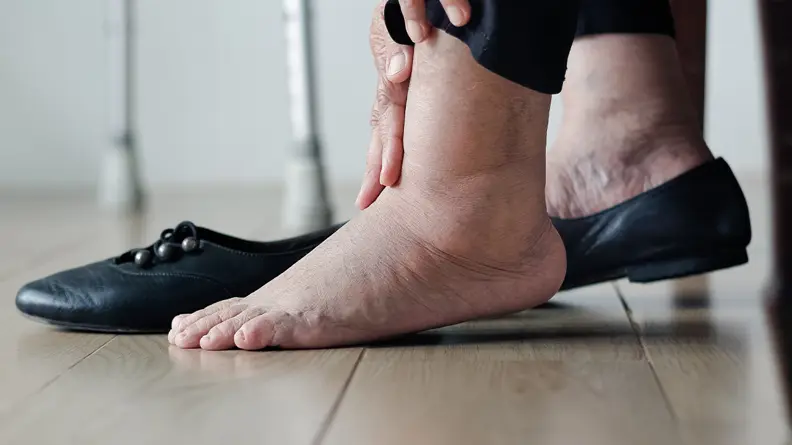
- Varicose veinsVaricose veins are a prominent indication of blood backflow. These veins appear enlarged, twisted, and bulging, affecting about one third of adults. Certain factors increase the likelihood of developing varicose veins, such as pregnancy, being overweight, or having a job that involves prolonged standing.
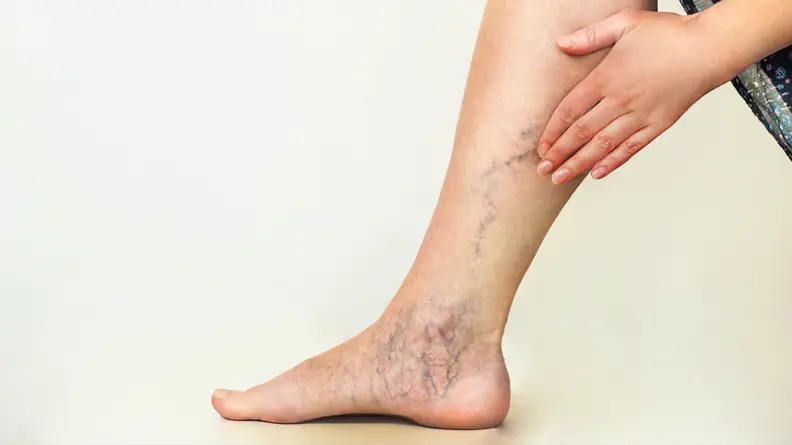
- Slow healing ulcersAround 80% of leg ulcers are associated with CVI. These ulcers tend to appear in the region between the ankle and mid-calf and can be notoriously slow to heal, often taking several months or even failing to heal completely.
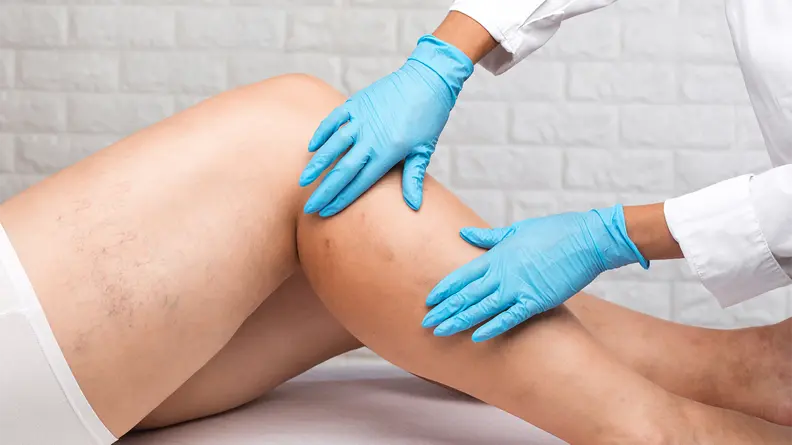
- Changes to the skinDiscoloration due to blood pooling is a common occurrence, with the skin appearing darker or developing red and brown patches. The increased pressure can also cause the skin to feel tighter, resulting in discomfort. Itching is another bothersome symptom experienced by many, and in some cases, CVI can even lead to the development of eczema.
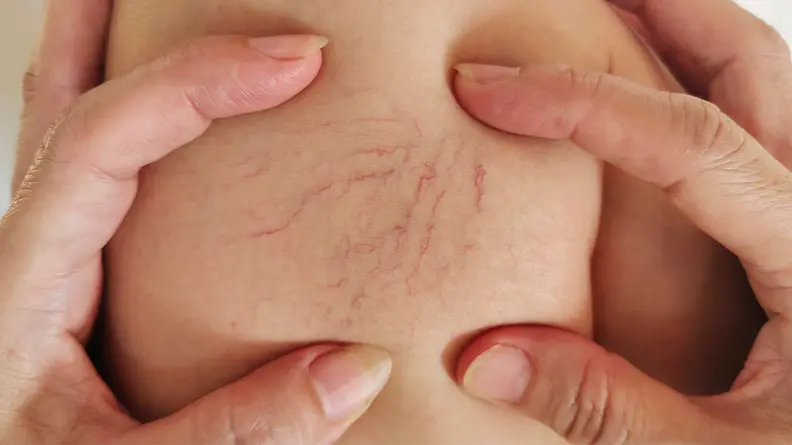
- Standing painA person with CVI may experience a ‘bursting and burning’ pain when first standing in the morning, this is caused when blood rushes at speed into the weakened veins. Also, a dull ache or heaviness can develop in the legs when standing.

- SwellingA common sign is swelling of the legs, particularly below the knee. This swelling can become more pronounced when sleeping in a seated position, as it contributes to increased blood pooling and may even lead to skin damage over time.

- SwellingA common sign is swelling of the legs, particularly below the knee. This swelling can become more pronounced when sleeping in a seated position, as it contributes to increased blood pooling and may even lead to skin damage over time.

- Varicose veinsVaricose veins are a prominent indication of blood backflow. These veins appear enlarged, twisted, and bulging, affecting about one third of adults. Certain factors increase the likelihood of developing varicose veins, such as pregnancy, being overweight, or having a job that involves prolonged standing.

- Slow healing ulcersAround 80% of leg ulcers are associated with CVI. These ulcers tend to appear in the region between the ankle and mid-calf and can be notoriously slow to heal, often taking several months or even failing to heal completely.

- Changes to the skinDiscoloration due to blood pooling is a common occurrence, with the skin appearing darker or developing red and brown patches. The increased pressure can also cause the skin to feel tighter, resulting in discomfort. Itching is another bothersome symptom experienced by many, and in some cases, CVI can even lead to the development of eczema.

- Standing painA person with CVI may experience a ‘bursting and burning’ pain when first standing in the morning, this is caused when blood rushes at speed into the weakened veins. Also, a dull ache or heaviness can develop in the legs when standing.

What can be done to treat the symptoms of CVI?
- Compression SocksCompression therapy plays a pivotal role in treating CVI. It involves using specially designed bandages or stockings that apply gentle pressure from the toes up to the knee. This compression aids in promoting blood flow towards the heart, enhancing the muscle pump action, and preventing swelling in the lower limbs. However, it's important to note that compression therapy is not suitable for everyone. Individuals with peripheral arterial disease, where the blood supply to the legs is already reduced, should avoid using compression therapy.

- Structured exercise and leg elevation“When on their feet, people with CVI need to be walking; when not walking they should be lying down or seated so that their legs are above the level of their heart. If less mobile, they should be encouraged to perform ankle exercises” writes Ruth Martin, leg ulcer specialist nurse.

- SurgeryWhen leg ulcers resulting from CVI become persistent and challenging to heal, a surgical procedure to remove the dead or dying tissue may be necessary to promote wound healing (3). Additionally, addressing the underlying cause, repairing the malfunctioning valves in the leg veins, can significantly alleviate the symptoms of CVI (4). In cases where these treatments prove insufficient, other minimally invasive options come into play. Injections or laser therapy can be utilised to seal and shrink veins that experience reflux (backward flow of blood). This procedure is less invasive compared to traditional vein stripping and can serve as an effective alternative.
- How can Revitive help relieve the symptoms of CVI?The Revitive Medic Circulation Booster has been shown to improve circulation in individuals with CVI (2), actively stimulating the leg and foot muscles, encouraging improved blood flow and circulation in the lower limbs. The key to this effectiveness lies in the innovative IsoRocker feature, which replicates the motion of heel-toe raises, gently mobilising the ankles without exerting excessive pressure.

- Compression SocksCompression therapy plays a pivotal role in treating CVI. It involves using specially designed bandages or stockings that apply gentle pressure from the toes up to the knee. This compression aids in promoting blood flow towards the heart, enhancing the muscle pump action, and preventing swelling in the lower limbs. However, it's important to note that compression therapy is not suitable for everyone. Individuals with peripheral arterial disease, where the blood supply to the legs is already reduced, should avoid using compression therapy.

- Structured exercise and leg elevation“When on their feet, people with CVI need to be walking; when not walking they should be lying down or seated so that their legs are above the level of their heart. If less mobile, they should be encouraged to perform ankle exercises” writes Ruth Martin, leg ulcer specialist nurse.

- Structured exercise and leg elevation“When on their feet, people with CVI need to be walking; when not walking they should be lying down or seated so that their legs are above the level of their heart. If less mobile, they should be encouraged to perform ankle exercises” writes Ruth Martin, leg ulcer specialist nurse.

- SurgeryWhen leg ulcers resulting from CVI become persistent and challenging to heal, a surgical procedure to remove the dead or dying tissue may be necessary to promote wound healing (3). Additionally, addressing the underlying cause, repairing the malfunctioning valves in the leg veins, can significantly alleviate the symptoms of CVI (4). In cases where these treatments prove insufficient, other minimally invasive options come into play. Injections or laser therapy can be utilised to seal and shrink veins that experience reflux (backward flow of blood). This procedure is less invasive compared to traditional vein stripping and can serve as an effective alternative.

- How can Revitive help relieve the symptoms of CVI?The Revitive Medic Circulation Booster has been shown to improve circulation in individuals with CVI (2), actively stimulating the leg and foot muscles, encouraging improved blood flow and circulation in the lower limbs. The key to this effectiveness lies in the innovative IsoRocker feature, which replicates the motion of heel-toe raises, gently mobilising the ankles without exerting excessive pressure.

- Compression SocksCompression therapy plays a pivotal role in treating CVI. It involves using specially designed bandages or stockings that apply gentle pressure from the toes up to the knee. This compression aids in promoting blood flow towards the heart, enhancing the muscle pump action, and preventing swelling in the lower limbs. However, it's important to note that compression therapy is not suitable for everyone. Individuals with peripheral arterial disease, where the blood supply to the legs is already reduced, should avoid using compression therapy.

Making Revitive part of your pain-relief plan.
While Revitive devices can provide symptomatic relief, it's important to remember that addressing CVI comprehensively requires medical attention.
Always consult with a healthcare professional to determine the most appropriate treatment plan for your individual needs.
Take the quiz to save an extra £10
Discover your ideal Circulation Booster - then try it risk-free for 90-days.